
Tackling the Antimicrobial Resistance Threat to Human, Animal, and Plant Health
Antimicrobial resistance occurs when bacteria, viruses, fungi, and parasites no longer respond to antimicrobial agents such as natural or synthetic drugs that kill or inhibit the growth of these organisms. Antimicrobials are medicines used to prevent and treat infections in humans, animals, and plants. They include antibiotics, antivirals, antifungals, and antiparasitics, and arguably rank among humanity’s most impressive achievements.
What happens when they no longer work? According to the World Health Organization (WHO), “as a result of drug resistance, antibiotics and other antimicrobial agents become ineffective and infections become difficult or impossible to treat, increasing the risk of disease spread, severe illness, and death.” If antimicrobials stop working because of antimicrobial resistance, common procedures such as hip replacement surgery could become deadly. A bladder or kidney infection could become life-threatening.
What causes antimicrobial resistance? The “misuse and overuse of antimicrobials are the main drivers in the development of drug-resistant pathogens,” reports the WHO. The resistance is also caused by a “lack of access to clean water, sanitation, and hygiene for both humans and animals; poor infection and disease prevention and control in health-care facilities and farms; poor access to quality, affordable medicines, vaccines, and diagnostics; lack of awareness and knowledge; and lack of enforcement of legislation.” What’s more, the resistance “occurs naturally over time, usually through genetic changes. Antimicrobial resistant organisms are found in people, animals, food, plants and the environment (in water, soil, and air). They can spread from person to person or between people and animals, including from food of animal origin.”
So, too many antibiotics are used unnecessarily and misused. The U.S. Centers for Disease Control and Prevention (CDC), for example, estimate that ,”about 47 million antibiotic courses are prescribed for infections that don’t need antibiotics, like colds and the flu, in U.S. doctors’ offices and emergency departments each year. That’s about 28% of all antibiotics prescribed in these settings.” This fact actually reveals ways to curb the resistance.
Indeed, each and every individual has a role to play to keep microbes from developing resistance to the drugs that fight them. It’s possible to use fewer antimicrobials and to use them more responsibly, which means taking antibiotics only when they are absolutely necessary: ask your doctor for an alternative when one isn’t needed.
So when is one needed? Antibiotics only help treat certain infections caused by bacteria, although some bacterial infections can get better without their use. The CDC states they should only be used to “treat serious, life-threatening conditions such as pneumonia and sepsis, the body’s extreme response to an infection. Effective antibiotics are also needed for people who are at high risk for developing infections.” Keep in mind that antibiotics do not work on viruses, such as those that cause colds, flu, COVID-19, most coughs, and sore throats. They won’t be effective either against polio, measles, chickenpox, mumps, rubella, hepatitis A and C, rabies, or herpes. So it’s very important not to pressure your doctor to prescribe an antibiotic and not to share or use leftover antibiotics.
Other simple measures can limit antimicrobial resistance. These include:
- Doing your best to stay healthy and keep others healthy
- Cleaning hands
- Covering coughs
- Staying home when sick
- Getting recommended vaccines, such as the flu vaccine
- Preparing food hygienically, following the WHO Five Keys to Safer Food (keep clean, separate raw and cooked, cook thoroughly, keep food at safe temperatures, and use safe water and raw materials)
- Choosing foods that have been produced without the use of antibiotics for growth promotion or disease prevention in healthy animals
- Eating healthy food ingredients and nutrients that have been demonstrated to enhance immunity, such as thyme, mushrooms, ginger, garlic, sage, zinc, echinacea, elderberry, andrographis and pelargonium
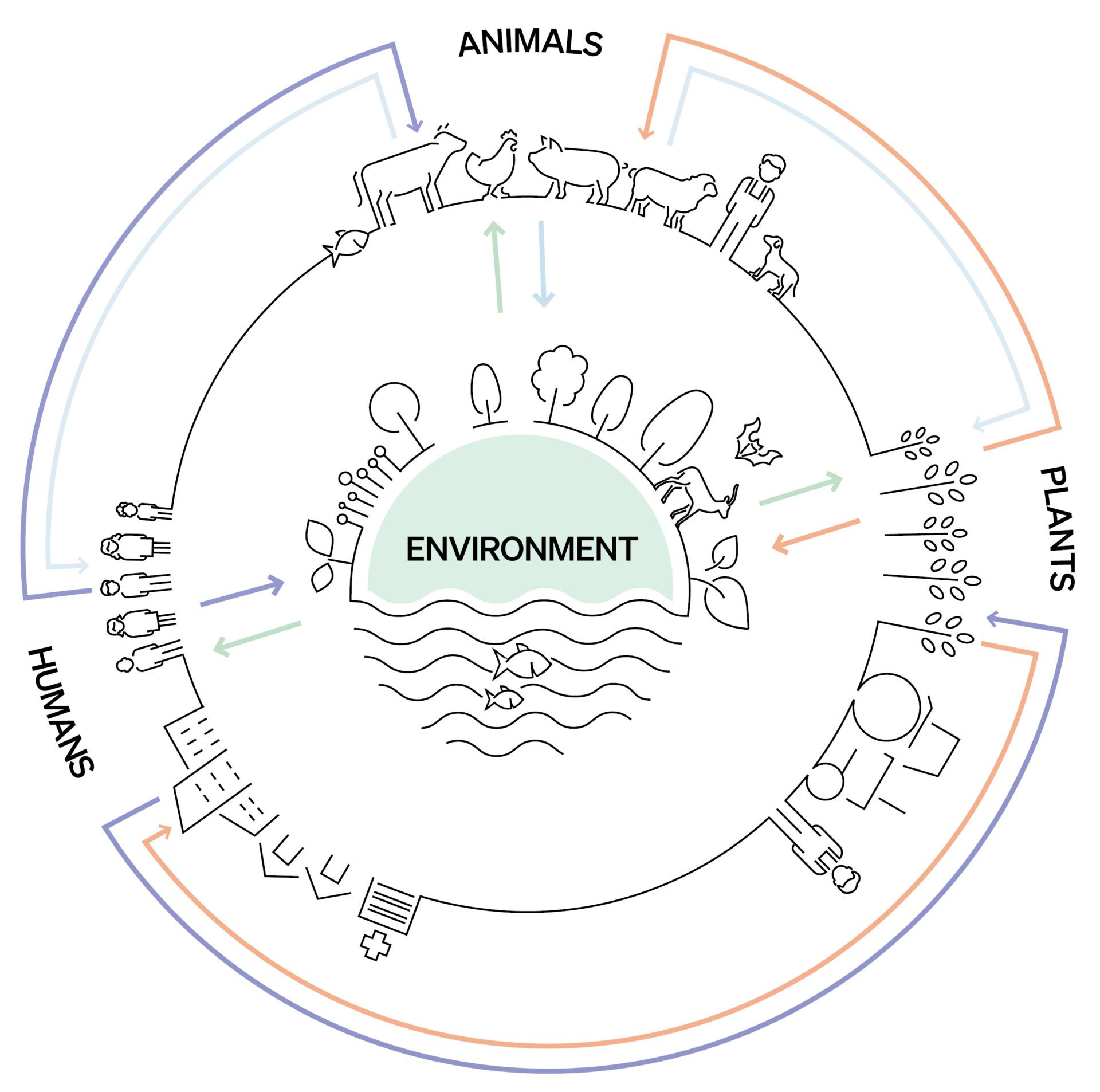
One Health – World Organisation for Animal Health (Source: WOAH)
To complicate matters, antimicrobial resistance not only affects human health, but also animal and plant health. The overuse or misuse of antimicrobials in one sector affects the other sectors. As the World Organisation for Animal Health explains, “Antimicrobials can spill into the soil and waterways, triggering the emergence of resistant microbes in the environment, which can in turn infect humans and animals. Resistant microbes can also spread from animals into the environment through manure, or from humans into the environment through clinical waste and sewage water.” Superbugs, which are strains of bacteria resistant to several drugs, can spread through the environment and between species.
This means measures need to be taken also to protect animals and the environment against the spread of antimicrobial resistance. These include:
- Being mindful of your animals’ health and welfare daily
- Vaccinating your animals
- Never giving antibiotics to your animals without a veterinary prescription
- Learning about the origin of the animal products you consume
- Demanding products from animals that are raised responsibly
Around 4.95 million deaths in 2019 were associated with antimicrobial-resistant infections, according to an article in the medical journal, The Lancet. The resistance is now a leading cause of deaths worldwide, higher than HIV/AIDS or malaria, as stipulated by the health resource testing.com. The WHO has asserted that antimicrobial resistance is one of the top 10 global public health threats that risks reversing the miracles of modern medicine. So do your part:
- Let your doctor know you understand the need to limit the use of antibiotics, and enquire about alternative options
- Increase the awareness of antimicrobial resistance by talking about the issue with those around you
- Celebrate World Antimicrobial Awareness Week (November 18-24)
- Ask your local authorities to address this serious challenge urgently
- Ask your national government to enforce laws regulating the sale of antibiotics
- Advocate to make antimicrobial resistance a globally recognized pressing issue

