New Twist on Older Cancer Therapy Leads to 100% Remission Rate
A cancer study sponsored by drug company GlaxoSmithKline has provided researchers with a surprising result: a 100% remission rate for the 12 participants.
All of the study’s participants had a very specific type of advanced rectal cancer – mismatch-repair deficient colorectal cancer – that, due to its genetic traits, made it a good candidate for this study.
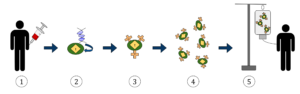
CAR T-cell Therapy, diagram by
Reyasingh56, CC BY-SA 4.0, via Wikimedia Commons
The study would have been an immense success even if it had only cured a few of them or had had lasting positive effects for all of them. That it sent all of the participants into remission is the first time this level of success has been found – the cancer was no longer detectable by an array of tests after the 8-month trial. And after a 12-month follow-up appointment, none of the 12 patients had disease recurrence.
According to The New York Times, Dr. Luis Diaz, author of the paper published in The New England Journal of Medicine and Head of the Division of Solid Tumor Oncology at Memorial Sloan Kettering Cancer Center, said: “I believe this is the first time this has happened in the history of cancer.”
Based on the older Chimeric antigen receptor (CAR) T-cell therapy, a type of immunotherapy that modifies the immune system of a person with cancer so it is more effective at finding and destroying cancer cells, this new therapy targets the protein, called PD-1 (programmed death-1), that keeps the immune system from attacking tumors. This protein forms a complex with PD-L1 (programmed death ligand-1) located outside of tumor cells. When this happens, it basically hides the tumor from the body’s immune system, allowing it to grow.
PD-1 ribbon, image by
Fvasconcellos, Public domain, via Wikimedia Commons
“This drug is one of a class of drugs called immune checkpoint inhibitors. These are immunotherapy medicines that work not by directly attacking the cancer itself, but actually getting a person’s immune system to essentially do the work. These are drugs that have been around in melanoma and other cancers for quite a while, but really have not been part of the routine care of colorectal cancers until fairly recently,” said Dr. Hanna Sanoff of the University of North Carolina’s Lineberger Comprehensive Cancer Center in an interview with NPR. She was not part of the study but has written about the results.
One famous case The Good Times wrote about in 2016 is the cancer treatment former US President Jimmy Carter received to fight melanoma, the drug Keytruda. Revolutionary at that time, that medicine is an example of immunotherapy that works by blocking the PD-1 pathway to help prevent cancer cells form hiding. Carter, who is 97 years old, remains free of the disease.
The therapy makes the PD-1 protein visible and the body’s immune system does the rest, without the need for chemotherapy, radiotherapy, or surgery. And the side-effects in the patients in this study were minimal, most commonly a rash or fatigue. This is a life-changing event as the various traditional therapies and surgery leave lasting physical and psychological scars on patients.
Researchers hypothesize that the discovery of this pathway could lead to other immunotherapies that inhibit PD-1 (PD-1 blockades), which would unlock the potential of T-cells to recognize and destroy cancer cells.
The results are encouraging, despite the small sample size. Significantly large trials and the collation of long-term data are needed as cancer management is a long-term undertaking.


This is GREAT news for those predisposed to this life threatening disease.
In this case the old adage “An ounce of prevention is worth a pound of cure” really does apply. A regular, albeit uncomfortable, regimen of colonoscopy screenings can detect most abnormal cell growth early enough to prevent the development of colorectal cancer in the first place. It is, however great to know that doctors now have new treatments for those that are not so fortunate.